At our team meeting last week, Freya, McKenzie and I were chatting about the common questions we get asked.
I decided to feature one this week for the blog – the hot topic of diagnostic imaging.
I think every patient we see (given the choice) would LOVE to see an image of their problem area.
I don’t mean pictures in a book – I mean pictures of themselves. An MRI scan usually.
It’s a common request – ‘Should I get a scan?’
Let me briefly explain the four most common imaging devices we use. I’m going to keep it simple 🤓.
Let’s start with the good old plain x-ray.
X-Rays
These are relatively easy to access, with GPs able to request them and some physiotherapists, like myself, who have done their IRMER training.
They are incredibly effective at producing images of bone. They are primarily used to show fractures or degenerative changes to a joint.
The positives are that they are quick and relatively cheap to produce and give good bone detail.
The main negative is that they produce ionising radiation, which can be harmful with too much exposure, especially to the young, and can cause cancers.
It is also a two-dimensional image with anatomical features superimposed over the top of the underlying ones. On a chest X-ray, for example, the ribs at the front will be superimposed over the spine at the back which makes it tricky to read. They also do not give us any information about the soft tissues.
The ionising radiation exposure risk is the primary reason we don’t X-ray everything. It’s always a balancing act between the benefits of the X-ray versus the radiation exposure. ☢️
Diagnostic Ultrasound
The next scan is a diagnostic ultrasound. This scan is exactly the same as the ultrasound scan you would have if you were expecting a baby. It is harmless and painless and uses sound waves to produce an image. These are very good at telling us more about soft tissues and show things like muscle tears, cysts, and superficial ligament sprains. They also allow us to look at a tissue whilst it’s being moved, which is really cool.
However, they are rubbish at giving us images of bone. The sound waves bounce off the bone, and it just shows up black on the scan.They are also very user-dependent.
CT scans (computer tomography)
CT scans also use ionising radiation to produce images. In a CT image, overlapping structures are eliminated (unlike in an X-ray), making the internal anatomy more apparent. CT scans can identify internal structures and see their shape, size, density, and texture. They are quick to perform and can give us information about a large area and a lot of detail about a small area. They produce much clearer images than X-rays.
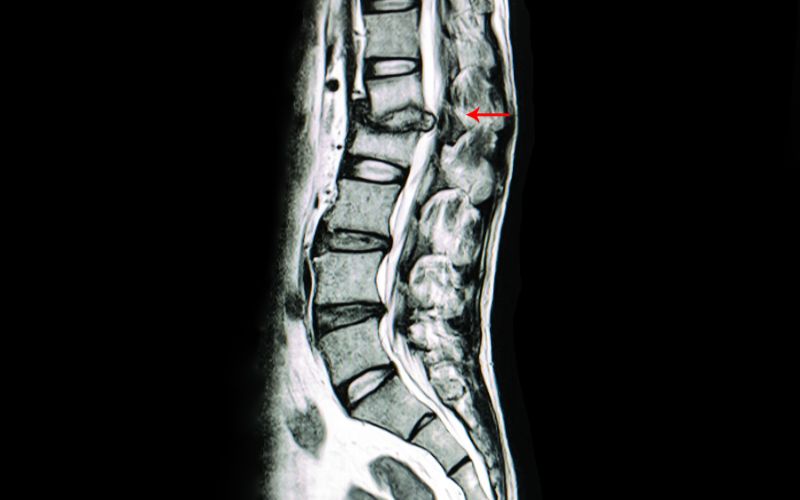
MRI scans (magnetic resonance imaging)
The big daddy of all imaging is the MRI scan. MRI provides better soft tissue contrast than CT and can differentiate between fat, water, muscle, and other soft tissue(CT is usually better at imaging bones).
The main benefit is that they do not use any form of radiation and are the imaging modality of choice when frequent imaging is required. However, MRI is more expensive than X-ray imaging or CT scanning. It is also poor at providing information about cortical bone.
The strong magnetic field created by the MRI scanner causes the atoms in your body to align in the same direction. Radio waves are then sent from the MRI machine, moving these atoms out of their original position. As the radio waves are turned off, the atoms return to their original position and send back radio signals. These signals are received by a computer and converted into an image of the part of the body being examined.
When should we use imaging?
So, given these scanning options, when would we use them? Answering this question is complex because every patient and every clinical presentation is different.
In general, if we suspect some bone pathology (fracture), we would probably choose a plain X-ray in the first instance. The downside is that if the fracture has just happened and isn’t displaced, X-rays don’t always pick them up. MRI would be more helpful but much more challenging to access.
If we suspect an Achilles tendon rupture or hamstring tear, these would be suitable for an ultrasound scan, BUT we don’t usually need the image to form a diagnosis.
If we want detailed imaging of bone, we would use a CT scan.
Suppose we want to look for a disc bulge, nerve root compression, bone stress injury or a detailed image of a soft tissue injury. In that case, we will use an MRI scan – but only under certain circumstances!
My concerns and thoughts
I am concerned about X-rays routinely performed on patients as part of an assessment. Simply:
- It is not worth the radiation risk.
- Anybody over 35 (and sometimes younger) will have normal, abnormal findings on X-ray. I am 44 and relatively asymptomatic, but I know that if you X-rayed my hands, wrists or neck, there would be some arthritic changes present. Does that mean I need to do anything about it? No. It is normal to be abnormal.
Over-imaging can be a real problem. Scans and X-rays WILL pick up abnormal things, but they could be normal for that person. Those things may not be causing the patient’s pain or problem.
I had a CT scan a few years ago for suspected kidney stones. I didn’t have kidney stones, but I did have a cyst in my liver.
Was it causing my problem? – no.
Did I need to do anything about it? – no.
Is it abnormal? – yes.
Did I need to know it was there? – no
As highly trained professionals, Physios do not need scans or imaging to form a clinical impression 95% of the time.
Believe it or not, we don’t always need to see inside to treat a condition appropriately. Many clinical tests tell us what’s going on without imaging.
I always ask myself, will it change what we do even if we get an image of this problem? For the vast majority of people, the answer is no; the management will remain the same.
Suppose I had concerns about a patient or they weren’t responding as I would expect in the timeframe I would expect. I may request a scan or refer to a consultant in that case.
In summary, imaging is advantageous if you pick the right one for the right problem – sometimes. Most people just don’t need them, and the risks can be too great with X-rays and CTs.
MRIs are the most useful to us but also the most expensive to access privately. Referrals on the NHS for MRI for routine problems are lengthy, and by the time the scan date arrives, the problem is either better or has deteriorated, or the clinical picture has changed.
I hope this helps explain the different types of scans and clears up the reasons we may or may not refer for them.
Best wishes
Charlotte